The Weill Cornell Department of Emergency Medicine at NewYork- Presbyterian Hospital is pleased to offer a postgraduate Emergency Medicine Residency for Nurse Practitioners. Our program is committed to educating NPs to become experts in the field of Emergency Medicine. Led by experienced Advanced Practice Providers and Weill Cornell’s renowned faculty, the Nurse Practitioner Residency provides our graduates with the knowledge and skills needed to deliver exceptional emergency care and to become leaders in our profession.
The Department of Emergency Medicine at Weill Cornell Medicine is affiliated with NewYork- Presbyterian Hospital. Located in the heart of New York City, we strive to deliver exceptional, compassionate, and equitable care to a diverse patient population across two hospital campuses: NYP-Weill Cornell Medicine and NYP-Lower Manhattan Hospital.
Across both campuses, the Department of Emergency Medicine serves over 140,000 patients each year. NYP-Weill Cornell Medicine is a Level I Trauma Center, Burn Center, Interventional Cardiology Site, and a Stroke Center of Excellence. Our goals are to provide the highest quality care to patients, offer an exceptional educational experience to students and residents, and engage in rigorous research to advance the practice of emergency medicine. In addition to the nurse practitioner residency, we offer residencies for physicians and physician assistants, as well as physician fellowships in Pediatric Emergency Medicine, Geriatric Emergency Medicine, Global Health, Healthcare Leadership and Management, and an Innovation Fellowship (offered in collaboration with Cornell Tech).
We are committed to excellence across all domains of Emergency Medicine. Faculty areas of expertise include toxicology, critical care, global health, international emergency medicine, geriatric emergency medicine, health care leadership and management, emergency medical services, disaster or resource-limited medicine, point-of-care ultrasound, medical informatics, telemedicine, medical simulation and education, and advanced airway interventions. Our Vulnerable Elders Protection Team (VEPT) is a first-of-its-kind ED/hospital-based multi-disciplinary team created to address elder abuse and neglect. We are a national leader in Telemedicine, including the inaugural launch of Emergency Department Telehealth Express Care and the Center for Virtual Care. As a New York State recognized Sexual Assault Forensic Examination (SAFE) Center, we provide comprehensive medical care and support to victims of sexual abuse.

Weill Cornell Emergency Department Faculty
As a nurse practitioner resident in the Department of Emergency Medicine, you will learn from, and work alongside, some of the brightest minds in medicine. Our physicians hold faculty appointments at the Joan and Sanford Weill Medical College of Cornell University, one of the top medical schools in the country. Renowned for their accomplishments in education and research, our faculty, along with physician residents, NPs, and PAs, sit on national committees, publish articles and book chapters, and regularly present at regional or national conferences. Faculty areas of expertise include toxicology, critical care, global health, international emergency medicine, geriatric emergency medicine, health care leadership and management, emergency medical services, disaster or resource-limited medicine, point-of-care ultrasound, medical informatics, telemedicine, medical simulation and education, and advanced airway interventions. All NP residents are invited to explore these areas, advance their learning, and collaborate with faculty on research or projects.
Established in 2015, the nurse practitioner residency prepares the nurse practitioner to become a competent clinician by developing skills in all aspects of emergency medicine while keeping the core nursing values of providing compassionate and empathetic care. The residency promotes the smooth transition from registered nurse (RN) to nurse practitioner (NP) who gains advanced skills, thinks critically, and works at the top of the scope of practice. The highly intensive 12- month curriculum is divided between the adult emergency department, pediatric emergency department (family nurse practitioners only), and multiple off-service rotations in key specialties. Every year, we accept between 2-4 candidates through a rigorous application and interview process. Applications are rolling, although starting January 1 they will start to be reviewed, interviews are held in April/May, and accepted candidates start on November 1 of the same year.

Nurse practitioner emergency medicine residents are employed by Weill Cornell Medicine with clinical appointments at New York-Presbyterian Hospital. For the upcoming cycle, the residency stipend is $75,700. You will also be covered for 1 year of your DEA License ($296). Residents receive medical, dental, and vision benefits, as well as 3 weeks paid vacation, $900 for CME expenses, and $296 for licensing-type costs. On-campus housing and parking are offered but subject to availability.
If accepted, the candidate must obtain the following prior to November 1st.
** Please keep in mind, hospital credentialing takes approximately 3 months to complete
To apply, click the link the Apply Now section
Interviews are held in April/May for the class starting on November 1st of the same year. Interviews will be hosted in person, with a zoom option.
We accept 2-4 Residents to each class.
Yes. We host two Open Houses in the spring to give applicants the opportunity to visit our department, meet faculty, and tour theinstitution. Please email ldm4001@med.cornell.edu if you are interested in attending for the dates.
The 12-month, 52-week, calendar encompasses over 2,300 hours of clinical experience divided between the adult emergency department, pediatric emergency department (for family nurse practitioners), and specialty off-service rotations. Below is the current curriculum, subject to periodic updates or revisions to best serve resident education.
| Orientation | 1 week |
| Vacation | 3 weeks |
| Adult Emergency Department | 25 weeks |
| Pediatric Emergency Department (FNP’s only) | 4 weeks |
| Medical ICU at Lower Manhattan Hospital | 4 weeks |
| Critical Care Triage Team | 1 week |
| Burn ICU | 2 weeks |
| Anesthesia | 2 weeks |
| Surgery & Surgical ICU | 2 weeks |
| Neurology | 2 weeks |
| Orthopedics | 2 weeks |
| Emergency Ultrasound | 1 week |
| Toxicology at the New York City Poison Control Center | 1 week |
| Elective | 1 week |
The residency begins with a classroom and simulation lab-based orientation, which introduces the Emergency Department’s electronic medical record, operating procedures, and workflow. Lectures and hands-on sessions cover fundamental emergency medicine topics such as splinting, suturing, EKG interpretation, and approach to the medical and surgical conditions commonly seen in the ED. The opportunity to obtain Advanced Trauma Life Support (ATLS) as well as the Sexual Assault Forensic Examiner (SAFE) course certification is also offered at this time.
Each resident is allowed to request three weeks of paid vacation during the residency. These requests are due at least two months before the start of the residency so that we can incorporate them into your block schedule.
Residents will rotate in the adult emergency department at both the Weill Cornell and Lower Manhattan campuses, and the pediatric emergency department at Weill Cornell (family nurse practitioners). Residents will evaluate and treat patients under the direct supervision of attending physicians as well as senior advanced practice providers. This close relationship provides an outstanding forum to learn from the diversity and complexity of medical conditions treated in the ED. Nurse practitioner emergency medicine residents also work collegially alongside physician residents and physician assistant residents, caring for patients of all acuity levels, including the most critically ill and injured patients. A typical work week involves an average of four 12-hour shifts. Each resident is expected to work a fair share of day, evening, night, and weekend shifts, as well as legal and religious holidays.
The majority of learning throughout the residency is clinically based and at the bedside, under the supervision of both physicians and senior advanced practice providers. Post-shift, nurse practitioner emergency medicine residents are expected to read independently to learn more about the specific diseases and patient presentations encountered that day.
The rotation schedule provides nurse practitioner emergency medicine residents with a solid foundation in clinical skills, knowledge, and procedures. We chose specialties that are most applicable to emergency medicine, with emphasis on critical care. When rotating through an offservice department, the residents serve as a full member of the sub-specialty team. Experiencing patient care from another specialty’s perspective provides residents with a broad understanding of the healthcare system and patient experience and allows residents to become more effective emergency providers. This experience also allows residents to meet the extraordinary members of other teams and form long-term professional relationships and connections.
Nurse practitioner emergency medicine residents are required to attend the daily Morning Report and weekly Wednesday Conference. Morning Report is an hour of education held before each weekday shift and is led by EM resident physicians. Typically, it includes either an interesting case presentation or a review of a specific topic. The weekly Wednesday Conference is taught by faculty from both Weill Cornell and Columbia University, as well as distinguished visitors from other institutions (Grand Rounds). It focuses on in-depth exploration of core EM topics. During rotations away from the ED, residents may also be required to attend conferences sponsored by the host department.
Additionally, APP residency leadership hosts monthly 4-hour call back days, which are protected learning hours focused on core EM topics including lectures, hands-on training and stimulations.
Our residents also attend several annual events hosted by our department over the year. This includes the Protected Airway Course where residents learn the latest advances in airway management and intubation, a Point of Care Ultrasound Course and our annual “Clinical Updates in Emergency Medicine” Conference.
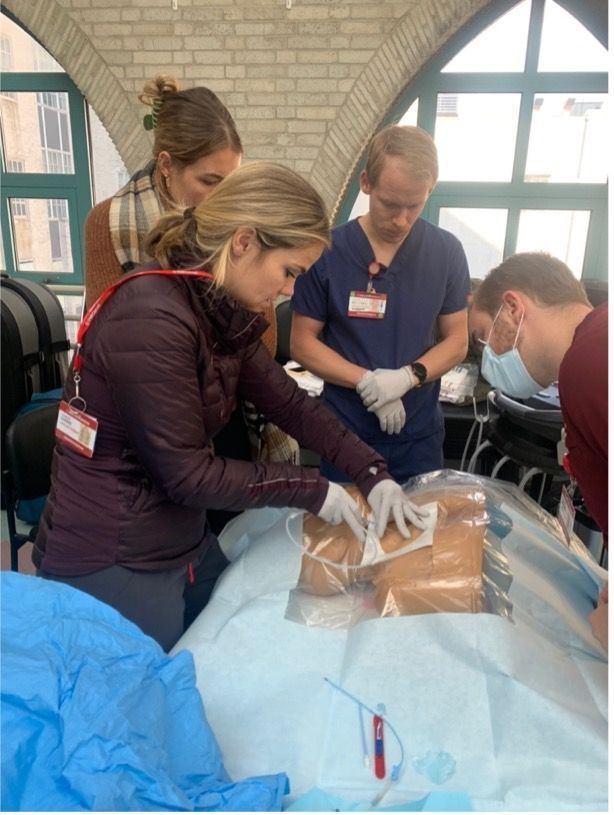
Central Line Placement at the Weill Cornell Simulation Center
Our residency works very closely with the Weill Cornell Medicine Simulation Center, which uses state-of-the-art equipment to teach critical procedures and practice resuscitation. ED faculty fellowship-trained in medical simulation guide our residents through realistic, hands-on training in a safe space. Simulation is a core component of all didactic opportunities, including Morning Report, Wednesday Conference, Callback Days, and other events.
Required in-service exams will be conducted three times over the course of the 12-month program. The content of these proctored exams covers foundational topics in emergency medicine and is designed to advance competency in this field.
Residents are encouraged to join us at the annual Society of Emergency Medicine Physician Assistants where we learn and network with other emergency PA / NP residents from across the country. One week of protected time is set aside in the schedule for this opportunity. Residents can use CME money to cover travel, lodging, and costs of conference.
One week of the residency curriculum is dedicated to an elective, where residents can explore a specialty or interest of their choosing. Optional electives include, but are not limited to EMS, Hematology/Oncology, Palliative Care, ED Administration & Leadership, Geriatrics, SIM.
We have a rolling application process until all interview slots are filled. Applications are reviewed starting January 1st for a November start date. We review applications until interview week, which is in early May.

Calvin Phung, FNP

Trisha Mae Magpantay, ACNP

Jasmin Lo, FNP

Natalie Giglio, FNP

Rebecca Ferneding, FNP, DNP

Helen Ting, FNP

Isabella Ryder, ACNP

Ivan Rodriguez-Carrillo, FNP, DNP

Alla Acevedo, ACNP

Karmay Hung, ACNP

Katherine Haley, FNP

Hollie Norman, ACNP

Shannon Scherer, FNP

Irina Kennedy, FNP (July Start)

Chris Clohessey, ACNP

Mollie Howard, FNP

Lauren Marks, FNP

Samantha Maione, ACNP

Murphy Neenan, FNP

Naomi Negita-Shak, FNP

Tara Mullen, FNP

Besiana Rugova, FNP

Alhaj Shah, FNP

Lauren McCue, ACNP

Chloe Pino, FNP

Alexander Wrynn, NP

Jasmine Johnson, FNP

Marisa Losavio, NP

Edyta Pedlowska, NP

Amy Barker, NP

Larisa Fridlyand, FNP

Hannah Claus, NP
Lauren McCue, MSN, ACNPC-AG

Lauren oversees all aspects of the residency program including education, curriculum, recruitment, and mentorship. She graduated from Rutgers University in New Brunswick, NJ with a BS in Biology in 2014. After graduation, she found her love of emergency medicine when she became an Emergency Department Patient Care Technician (PCT) at Trinitas Hospital in Elizabeth, NJ. While working there, she finished her nursing prerequisites and applied to nursing school. She attended Massachusetts General Hospital’s Institute of Health Sciences in Boston, MA where she obtained her BSN and MSN in Acute Care. While in graduate school, she worked as an emergency department registered nurse (RN), reconfirming her passion for emergency medicine. After obtaining her graduate degree as an acute care nurse practitioner, she was accepted into the NYP-WCM NP EM Residency Program in 2019. She has been actively involved in teaching, mentoring, and precepting NP students. In 2022, she was awarded Columbia University’s School of Nursing Preceptor of the Year in Acute Care. She is a steadfast advocate for our Victim Intervention Program and volunteers her time providing care and support to victims of sexual, domestic, and physical assaults.
Lauren McCue, NP
Director of ED NP Residency Program
ldm4001@med.cornell.edu